Chorioamnionitis is not a word I ever planned on learning to define based off of personal experience. But one year ago today, that is exactly the reason that my Virginia May was born, 8 weeks premature. My first two healthy babies were born at 41+ weeks, and I was on-track for another healthy, active, full-term pregnancy. That is, until I wasn’t.
I could write a novel of all of the tiny little details I remember from that pregnancy, that weekend, that day. But I won’t bore you with that. Today, I’ll just look back and remember the numbers and moments that stood out most to me, and explain the story of how my little miracle baby got here, in spite of the odds.
First, some facts:
- 40 weeks: Average length of a human pregnancy, although “full-term” is defined as anywhere in the window of 37-42 weeks, with the ideal being between 39-41 weeks.
- 32 weeks: One of the milestone ages that baby’s in utero reach where they are expected to have a very high chance of survival and a normal life after birth, although they will possibly need some assistance with breathing and feeding initially.
- 32 weeks 5 days: The gestational age Virginia was born.
I was fit. I was strong. I was healthy. I was doing “all the right things” to make this my best pregnancy and delivery. At my 32 week checkup just 5 days before, everything looked perfect.
Until Mother’s Day weekend. I won’t give you the play-by-play, but there were more than a few moments that I thought… hmm… something might be off? Yet I am so GRATEFUL that despite these nagging fears in the back of my mind, my family got to have a wonderful time together that weekend doing things we love, blissfully unaware that things were about to get crazy.


So here’s how it went down after that:
Monday, May 11, 2015:
8am: Wake up and wrangle 2 year old son at his Occupational Therapy appointment. Meanwhile, I’m noticing that my “Braxton Hicks” are kinda sharp. And maybe coming more often? I don’t know, but I’m too busy focusing on my other two kids.
10am: Visit daddy at his office and go to Library story time, struggling to hold my son during these contractions. Yeah, definitely weird. We leave story time early so I can go lay down on the couch, chug some water, and start paying attention to my body.
12pm: Contractions are 10 minutes apart, sometimes less, for an hour. I am now fully committed to resting, and if I can’t get them to calm down, I decide I’m calling my OB. But after a couple of hours things subside. I turn on Netflix and we spend the rest of the day resting.
7pm: Put the kids to bed. Make a point to tuck them in myself, although I had not been doing that as much because my body was just sore and tired. But for some reason, I felt strongly like I should make sure to come and kiss and cuddle each kid that night. Then I went to bed myself.
10pm: Wake up to contractions coming with a vengeance. 6-8 minutes apart. I am lying there cringing with the thought of the next wave hitting. This isn’t normal, I think. But I don’t want to be “that person” who shows up at L&D over Braxton Hicks! Especially since I’ve never had any issues in the past, and my recent checkup was fine! (Which is stupid. That’s their job, to check you and make sure everything is fine if you don’t feel fine. Don’t be like me.) I pray for a sign.
11pm: I go to the bathroom and there’s a sign: I’m bleeding. I spring into ACTION. Wake Mike. Call for a babysitter. Call my OB. Call my mom. Call my doula, Erica. Grab my bag. Hop in the car. Drive into the peaceful, dark night. Enjoy the still, quiet, calm ride, focusing on my body and my baby.
Tuesday, May 12, 2015:
12am: Arrive at L&D. Get hooked up to the monitor. First contraction hits. Baby’s heart rate is TANKING. I sit straight up in bed and say, “Is THAT my BABY?!” “Yeah… and if it doesn’t pull back up in a second you are getting prepped for the OR, honey,” concerned nurse says, her eyes not leaving the monitor.
Things happen fast now: Oxygen, an IV, Magnesium Sulfate (to stop the contractions, and makes me feel like a fire breathing dragon), a big needle is jabbed in my leg (steroids for the baby’s lungs, makes me feel like my heart is racing), an internal exam (4cm, bag of waters bulging), ultrasound (fluid levels are on the low end).
I am terrified and I say so.
They are able to get the contractions to slow and the baby’s heart rate is not dipping as bad and is always picking back up, but I’m told I have just been admitted for the duration of my pregnancy. The hope is 24 hours until delivery. It would be fantastic if we make it even longer.
3am: I am settled into my room. We send Erica home. I try to sleep but I can’t. Sleep is like this black hole, and I am afraid to surrender to it. I am afraid if I do, I won’t come back, or worse, my baby won’t come back. That I’ll get lost in sleep land and forget to keep my baby alive. I am afraid to move in case my water breaks. It’s unnerving, terrifying, and I feel terribly alone.
9am: My doula comes back to give Mike some time to arrange things at home. The morning is a blur of tests. Nobody knows why I am in preterm labor. Nobody knows why my baby doesn’t like the contractions. These are the strongest possibilities:
- Pre-eclampsia (24 hour urine sample started)
- Infection (blood tests run)
- Intrauterine Growth Restriction- IUGR (bio-physical profile completed)

Nothing is clear and nobody can tell me when, why, where, or how. Which is petrifying to me. I can do labor, but I can’t do THIS. Neonatology comes in to tell me what to expect from a (very likely) premature delivery:
- Baby probably will need help breathing.
- Baby probably will need help eating.
- I won’t get to see my baby at the birth.
- My baby will be taken straight away to the Special Care Nursery (a level 2 NICU).
- My birth desires are all out the window.
The Plan: Bump the second dose of steroids up from 24 hours to 12 hours (~2pm), schedule a cesarean for 6pm. Relief floods me knowing that I won’t have to endure another night.
One of my biggest desires had been to be the one to announce the sex of the baby at birth. This was the first pregnancy where I had not found out the sex ahead of time, and I really wanted this special thing. It was the one thing I had on my Birth Plan that could follow me no matter whether I had a vaginal birth or cesarean birth. Except, I didn’t plan on a preemie cesarean birth.
The ultrasound tech offered to come back to see me and quickly check the baby’s sex, write it on a piece of paper, fold it up, give it to Erica, who would show it to me the minute my baby was born in the OR so that I could announce it anyway. It was the smallest gesture, but it meant so much to hold on to at least one little tiny thing.

I ask for something to eat, and I can’t because, surgery. They feel bad, though, so they break the rules, and let me have a popsicle. “Maybe it will perk the baby up, too,” they say.”Maybe things will turn around and we can cancel the cesarean,” they say. I am hopeful. I am grateful for this tiny thing.
11:45am: Mike is back, and with things settled down, we send Erica home again, to return for the pre-op and cesarean later. We spend some time just the two of us talking.
“If it’s a girl, let’s name her Virginia May,” my husband says. Yes, let’s. (If she was a he, I don’t know what we would have done, we had no name planned.)
12pm: The nurse walks in. “Is she still dipping her heart rate, I haven’t noticed any.” I say. “Yes, she is.” My heart sinks. I suddenly feel like we made a mistake sending Erica home. I tell Mike to text her to come back.
My nurse is on the phone with my OB, who is back at his office seeing patients for the day until it’s time for my cesarean. “Yes, things are just….” she cuts off. “I need to call you back, we’re having a decel.” She hangs up.
Oxygen mask.
6 people flood the room.
Some of them are in surgical scrubs.
This is it.
I know.
Exam. Still 4cm.
“Keep breathing.”
Shave.
“CODE RED IN O.R. ONE,” a nurse pages.
They run. We crash into, ironically, a crash cart, in the hall on the way out.
Mike is left behind.
“We’ll plug the monitors back in in the OR and if the heart rate is back up, we’ll stop.”
I squeeze my eyes shut. I keep breathing. I tell her we hear her and we are coming, fast. I tell her to hold on. Please hold on baby, please hold on. Please don’t go. Please. We’re coming.
My bed is slammed into the OR bed.
Frantic discussion about raising my bed to match the height.
I notice the monitor cords are trapped between beds, and lean over to get them and hand them off. Plug them in fast, I pray.
I try to stand up to get myself in the bed. They roll me.
The nurse is plugging them in and staring at the screen. Still that slow, ominous heart rate.
People are running around crashing into things and trying to get organized, calling out orders to each other. It’s practiced chaos.
I have a scary fleeting thought: These are just people. Regular ordinary people, with training and skills, but still, just human. There is no magic here. Nobody knows the outcome.
Please knock me out now. It is maybe 2 minutes, but it feels like forever.
Finally they are all in place. Pressure on my throat, and then I’m gone, into that seductive blackness. Finally I let go.
I am not awake, I am dreaming. Happy dreams, I don’t remember. Mike is pacing anxiously in my hospital room, waiting. I am not there to see, but later I hear what happens:
She’s pulled from me at 12:13pm. Limp, blue, unresponsive, surrounded by meconium (her own poop, that she amazingly didn’t breathe in). An APGAR of 1 (out of 10). All she had left of life was a weak pulse. In his hurry, the head of Obstetrics calls her a boy. It gets entered into the computer, and her first baby bracelets say, “Rich Baby Boy.”
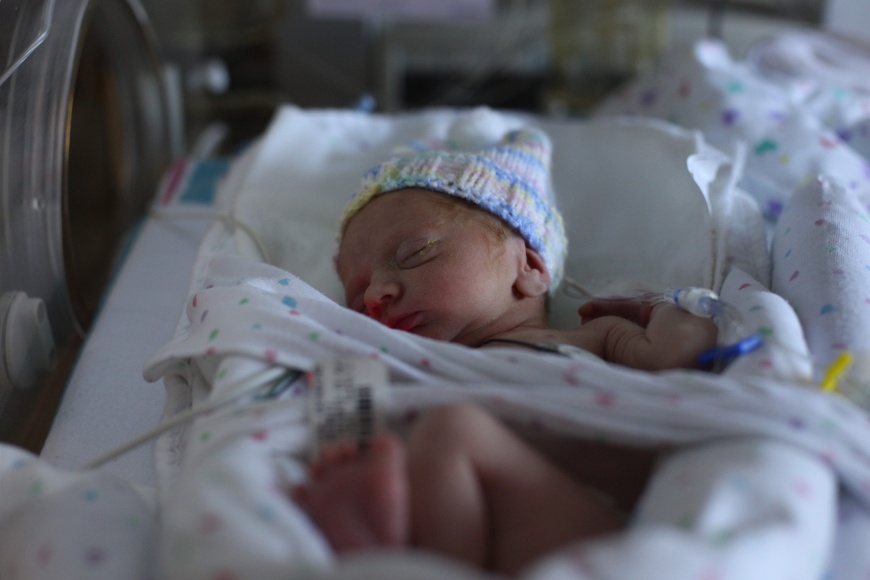
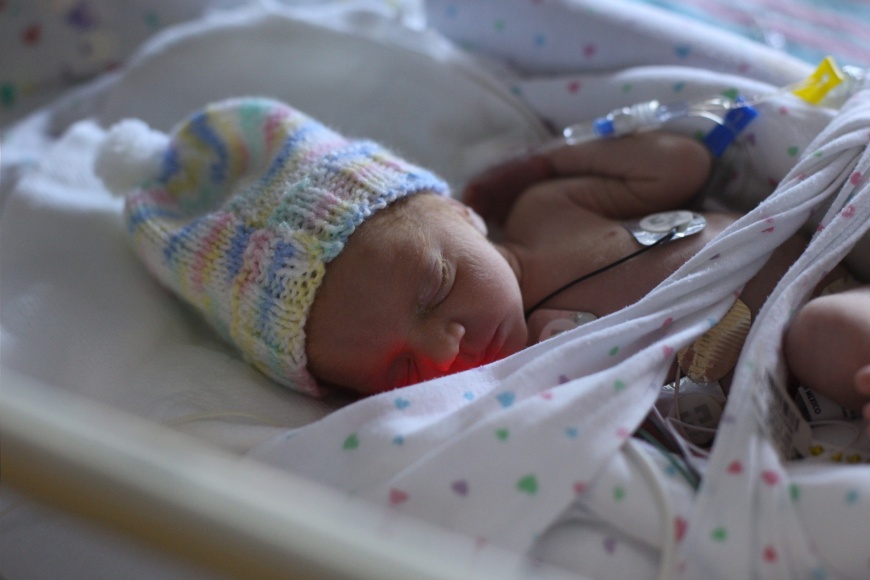
They work to resuscitate her. Nurse Robin, from the Special Care Nursery, who I will later get to know, is there. She sees my baby in these first moments. Sees her take her first breath. Turn back from the edge of that black hole. Back to the light. Begin to turn pink. Cry. Five minutes later, her APGAR is a very healthy, normal 8.
They tell Mike, “We think you might have had a boy. We aren’t sure, though. But he’s going to be ok!” Relief.
A little bit later and he is allowed to walk with her as she is transported in her isolette from the OR to Special Care. And they confirm: she’s actually a she. And she’s breathing. She’s looking around. She’s OK.


Meanwhile my OB has made a frantic dash from his office to the hospital. He arrives in time to take over putting me back together. My abs are sore for days later, and I wince just imagining why.
I awake in Recovery. I am in pain. The first thing I ask is if my baby is ok. I still don’t know she’s a girl. They tell me she is and I am flooded with relief. I can cope with anything after that. I ask for morphine every five seconds. It takes them forever to bring it to me. Erica sits and we talk and I am so grateful to talk about her life and things outside these walls. She shows me the piece of paper. It’s a girl. I knew. I love her already.
My mom arrives.
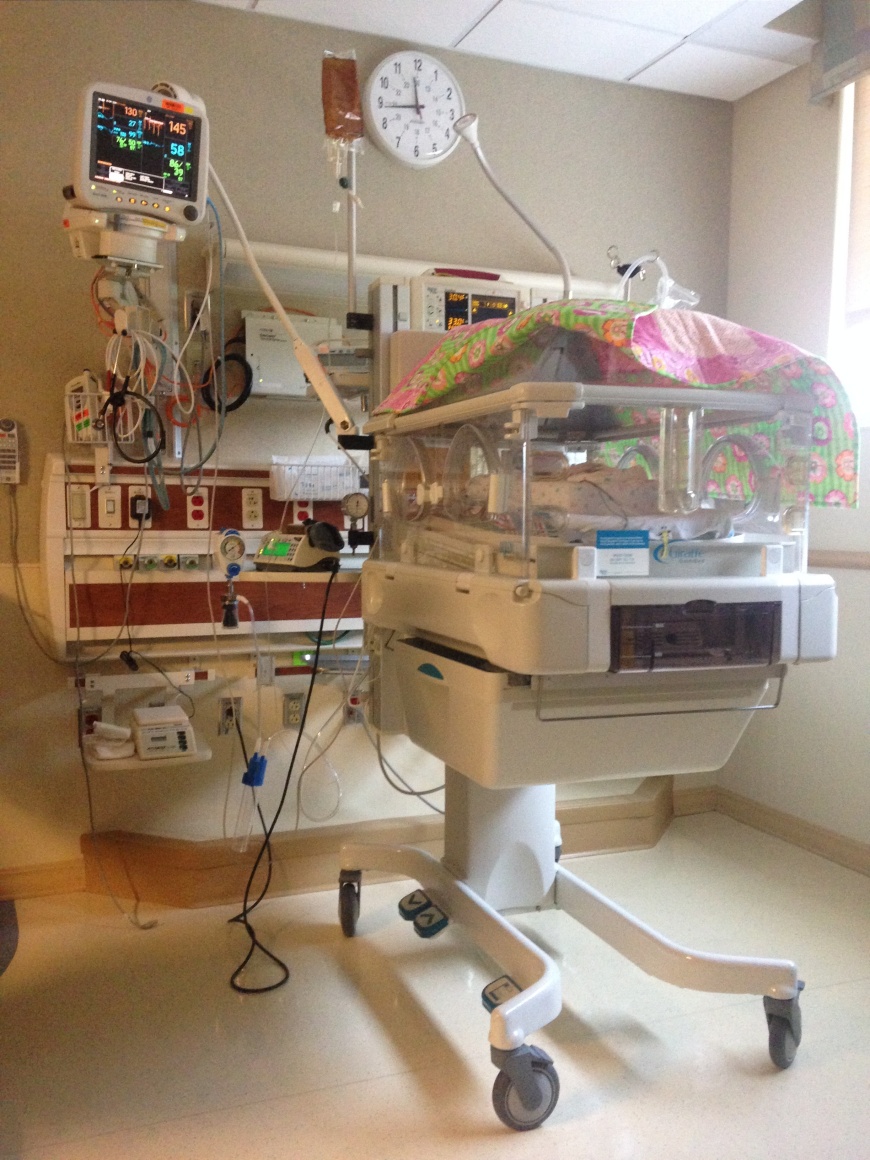
Two hours go by and they wheel me to her room to see her for a minute. I don’t remember seeing her. Just the machines and wires. I am out of it.
I am taken a floor below and a long hallway away. To Postpartum.

Mike doesn’t leave her side.

12 hours later I am allowed to get up for the first time. I stand. I shuffle into a wheel chair. They wheel me upstairs a little after midnight. I gently lay my hand on her, like they tell me to do to not disturb her but let her know I am here. She’s tiny. She’s perfect. I love her so much.

I go back to my room and sleep. And then wake at 3am and bawl my eyes out while pumping, alone in the darkness. When the kind nurses come in and ask me how my baby is, I instinctively reach to my stomach. And then I remember she’s not there anymore.
It is 24 hours after her birth and I get to hold her for the first time. It’s heaven.

She latches on to nurse. I am amazed. Nothing else can phase me. Not the bilirubin lights, not the feeding tube (put in that second night), not the IV lines, not even having to spend time apart. I know she will be ok.

The rest of her stay is:
- 8 Days: The number of days that I am in the hospital and I don’t get to see my other two kids. 5 days as a patient, and 3 days as a “Bethesda Inn” resident, a program that allows mothers with a baby in the Special Care Unit to live a little longer in their hospital room after discharge. My other two “meet” her by FaceTime first.

- 17 Days: The number of days she lives in the hospital.

- 1: The number of “friends” she makes. There is another baby girl two doors down whose mother and father are also always there. The four of us parents talk in the Family Lounge when we are eating. I am grateful for a friend.
- 2-3 hours: The amount of time in between each pumping session, around the clock. It’s so hard to force myself awake in the middle of the night to pump with no baby to rouse me. The first night, I resent the sounds of the crying babies in other rooms. I ask my nurse to tell the mothers to do something about it. I am drugged and out of it, but I realize even as I say it how ridiculous it is.


The placenta pathology report comes back. I had an infection. Chorioamnionitis. A bacterial infection that was ravaging the placenta, the amniotic sac, and the cord, the literal lifelines to my baby. It was traveling its way down the cord to her. That is why she let go. We we were fortunate to be in the hospital when it happened: when my placenta shut down and stopped delivering oxygen to her. Only a few more minutes, she would have been brain damaged, as 25% of babies affected by chorio are. A few minutes more after that, she would not have survived. Another 25% of babies do not. We are lucky. She’s perfect.


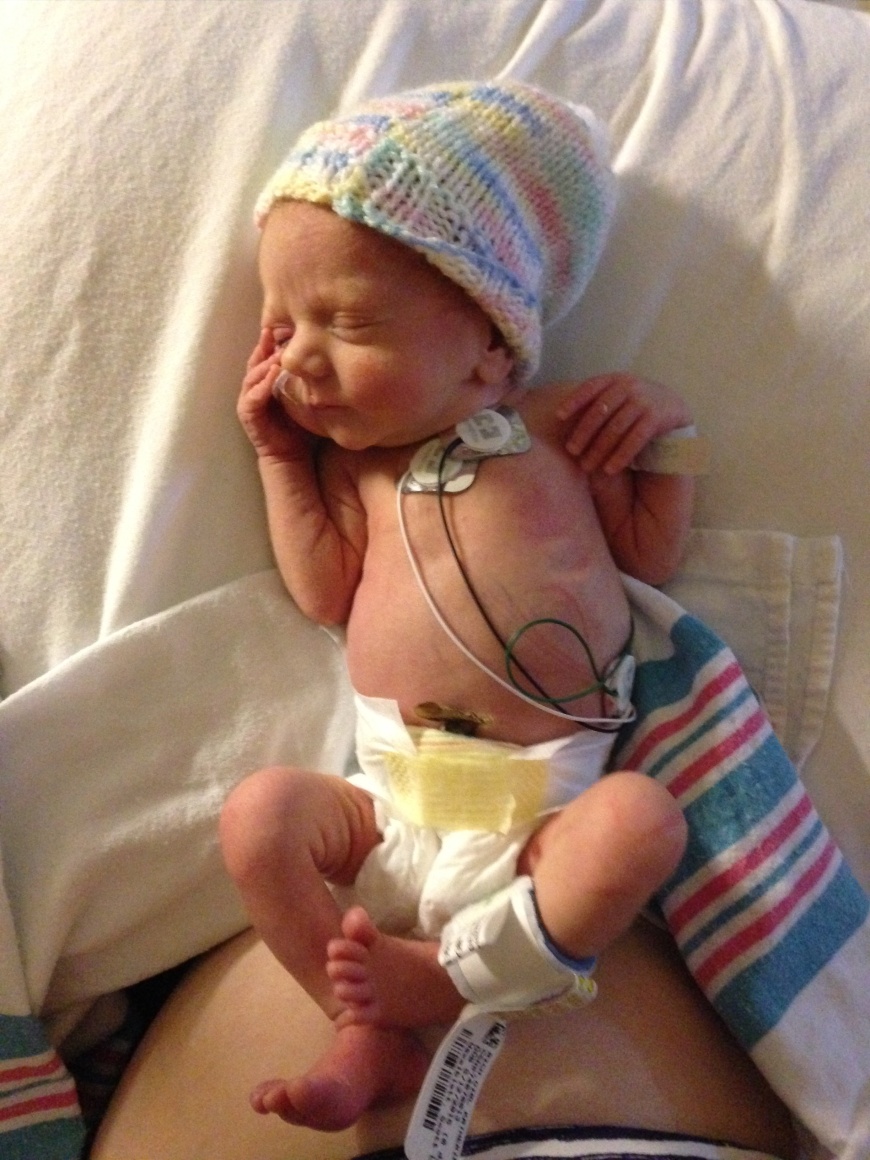
We spend time skin-to-skin as much as possible. We are waiting for her to grow. After 3 days on antibiotic via IV, we are cleared. We are officially out of the woods. She will be ok. She never needed help breathing after those first few minutes. She was able to latch and transfer milk from the beginning, she just needed the tube to giver her time to grow strong enough to do it regularly.

The only other person we let see and hold her is my mom. I’m too afraid of germs. I don’t want to overstimulate her. I want her to be in a quiet and peaceful environment and focus on growing. Not being talked to or over. Not being held and passed around. She should still be in my womb, in darkness, sleeping the majority of the time, rapidly growing. She’s not, so we have to recreate the womb outside me. Her new womb is a hospital room. Before I nourished her via a cord that connected us, now we are connected by a long hallway. There will be time to get to know her and show her off later, when she gets to the age she would have been born.

 Instead of milestones like: first smiles, first rolls over, etc. her first milestones are:
Instead of milestones like: first smiles, first rolls over, etc. her first milestones are:
- Holds her own temperature and graduates from being in a covered isolette to being in the “open air.” She has to hold her temperature herself to go home.
- Taking increasing amounts of her feedings via bottle instead of the tube. She has to take all of her feeds 100% by bottle for one day before she can go home.
- Gaining weight. She has to be at least 4lbs and gaining to go home.
- 35 weeks. She has to be at least 35 weeks gestation to go home.


Her cheeks get fat first. Then her belly and legs.

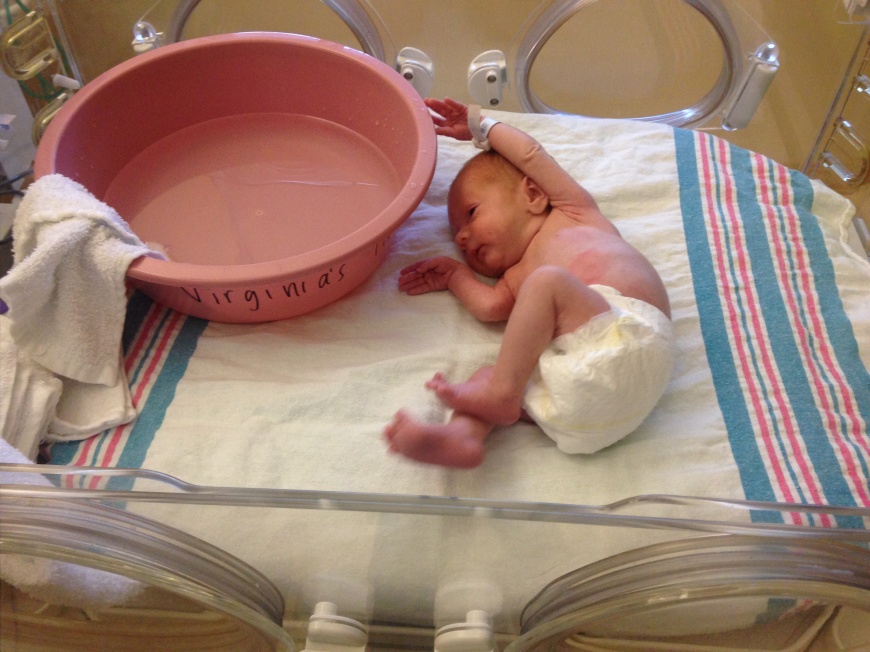
She grows. She becomes more alert. I ask if she will ever become a normal baby, and they assure me that yes, she will. And on May 29th, 2015, I can hardly believe it when they unhook her wires and monitors, let me put her in her carseat, and walk out the doors.

It feels like a jail break. The kids meet her in the lobby for the first time in real life.


And that is just her beginning.
